 
Moreover, some works have been published on the possibility of coupling microscopy and microfluidics for diagnostic applications. Several experimental and numerical studies have analyzed the behavior of RBCs and their relation with the viscosity of whole blood using microfluidics. The rise of microfluidics in the past decades has opened alternative methods to measure the rheological properties of fluids, including blood. The viscosity of blood depends highly on its red blood cell (RBCs) concentration and biomechanical properties, such as aggregation and membrane elasticity. This characteristic of blood is known as shear thinning, which is the property of some complex fluids to decrease their viscosity as the shear rate increases (e.g., increasing its flow velocity), and it has been widely observed in blood. The rheological properties of blood have been studied for many years, and it has been clearly demonstrated that blood has a non-Newtonian behavior. By means of these normalization methods, we were able to determine the differences between the red blood cells of the samples and define a range where healthy blood samples can be described by a single behavior. The proposed methodology is able to predict the health conditions of the blood samples by introducing a non-dimensional coefficient that accounts for the response to shear rate of the different donors blood samples. In this work, we present two methods that successfully normalize the viscosity of blood for a single and for different donors, first according to the concentration of erythrocytes and second according to the shear rate. Using an experimental analysis of the interface advancement of blood in a microchannel, we determine the viscosity of different samples of blood. These properties affect the viscosity of blood as well as its shear thinning behavior. You would not then need any further tests.The rheological properties of blood depend highly on the properties of its red blood cells: concentration, membrane elasticity, and aggregation. If it has been raised by a recent infection (a very common cause) then it is likely to return to normal when your infection improves. However, before you have further tests, your doctor may suggest that you have the ESR, CRP, PCT or PV test repeated after a period of several weeks or months. It is not usually possible to make a diagnosis of a certain condition just from a raised ESR, CRP, PCT or PV level. PCT is more specific for pneumonia and sepsis and is used to support a possible diagnosis to enable treatment to start quickly. This may prompt a doctor to do further tests to find the cause. A raised ESR, CRP, PCT and PV may indicate that some inflammatory condition is likely to be the cause. For example, you may be unwell but the cause may not be clear. In other words, a raised level means that 'something is going on' but further tests will be needed to clarify exactly what that is. When are these blood tests used? To help diagnose diseasesĮSR, CRP, PCT and PV are nonspecific tests. PCT is more sensitive than CRP so is a better marker for sepsis. Procalcitonin levels are only used for pneumonia and sepsis. It is also lowered in conditions where your body has lower protein levels - for example, in some liver or kidney diseases. Some conditions lower the ESR - for example, heart failure, polycythaemia and sickle-cell anaemia. 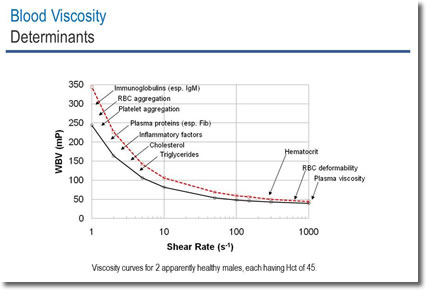
Crohn's disease (inflammatory bowel disease).Some cancers - for example, myeloma and Hodgkin's lymphoma.Various muscular and connective tissue disorders that have chronic inflammation as a feature - for example, polymyalgia rheumatica, giant cell arteritis or systemic lupus erythematosus.Certain infections (mainly bacterial infections).PV, however, is more sensitive and more specific than either ESR or CRP when monitoring the activity of rheumatoid arthritis.ĮSR, CRP and PV can be raised in many inflammatory conditions - for example: CRP is not affected by as many other factors as the PV or ESR, making it a better marker of some types of inflammation. Generally, PV and ESR do not change as rapidly as CRP does, either at the start of inflammation or as it goes away. Raised ESR, CRP and PV levels are all markers of inflammation. What conditions affect the erythrocyte sedimentation rate and C-reactive protein level? 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
